As medical marijuana use continues to rise nationwide — especially among adults who already take multiple prescription medications — understanding how cannabis interacts with common prescriptions has never been more important. Today, nearly half of U.S. adults take two or more daily medications, and many add cannabis for pain, anxiety, or sleep support. But drug interactions can be serious, because they occur when one substance changes the way another works in your body.
What are cannabis drug interactions?
Cannabis drug interactions occur when THC or CBD changes how prescription medications are metabolized, potentially increasing or decreasing their effects.
In plain English, a drug interaction means a medication may become too strong, too weak, or behave unpredictably when combined with something else — including THC or CBD. That’s why patients should never self‑experiment or guess their way through combining cannabis with prescription drugs; professional guidance is essential for safety..
Considering medical marijuana? Start with a risk‑free consultation.
Medical marijuana interacts with the body through the endocannabinoid system (ECS), but it also interacts with the CYP450 enzyme system, which is responsible for metabolizing most prescription drugs. Because of this, cannabis can increase, decrease, or delay how certain medications work. These effects vary depending on whether the patient is using THC, CBD, or a combination of both.
Why Cannabis and Medication Interactions Matter for Patient Safety
Drug metabolism is the process your body uses to break down medications so they can be used safely and effectively. Most of this work happens in the liver, which acts like a processing center — sorting, breaking down, and clearing substances from your bloodstream.
Inside the liver, a family of enzymes called CYP450 handles the majority of medication processing. Think of CYP450 enzymes like traffic lanes on a busy highway. Each medication needs a lane to move through. When cannabis — especially CBD — enters the system, it can slow down certain lanes, block them, or force other medications to merge, creating a “traffic jam.” This can cause medications to build up in the bloodstream or clear too quickly.
This is why medical marijuana drug interactions matter: if THC or CBD slows down the enzymes responsible for metabolizing your prescriptions, the medication may become stronger, longer‑lasting, or more sedating than intended. Understanding this helps patients use cannabis safely and confidently.
THC Drug Interactions: What Patients Should Know
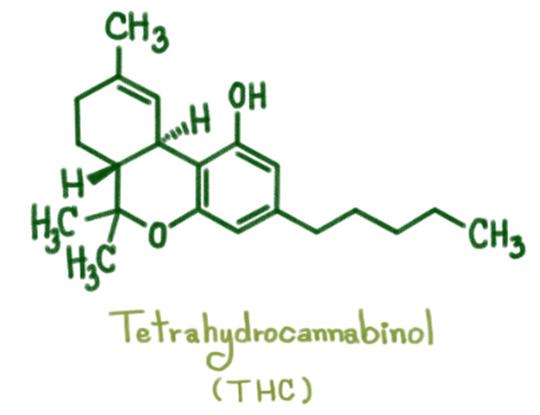
THC (tetrahydrocannabinol) is the cannabinoid most associated with psychoactive effects. It binds to CB1 receptors in the brain, influencing mood, perception, and pain signaling. But THC also interacts with medications through the CYP450 system — particularly CYP2C9 and CYP3A4.
How THC Causes Sedation
Common medications that may interact with THC include:
- Blood thinners (e.g., warfarin)
- NSAIDs
- Opioid pain medications
- Benzodiazepines
- Certain antidepressants
- Sleep medications
Because THC can enhance sedation, patients taking benzodiazepines, opioids, or sleep medications may experience stronger effects. THC may also alter the metabolism of blood thinners, potentially increasing bleeding risk.
Real‑World Example of THC drug interactions:
- Taking THC + Xanax may amplify drowsiness, impair coordination, and increase fall risk.
- THC + opioid pain medications may intensify sedation and slow reaction time.
- THC + sleep medications can lead to next‑day grogginess.
Dose Matters
Clinical studies suggest that a small THC dose may have mild interaction potential, while higher doses — especially edibles — can significantly increase sedation or alter medication metabolism.
Who Should Be Most Cautious
- Older adults
- Patients on multiple sedatives
- Anyone taking blood thinners
- Patients with heart conditions
.Learn how THC fits into a safe treatment plan.
CBD Drug Interactions: Why CBD Requires Extra Attention
CBD is often misunderstood as “completely safe” because it’s non‑intoxicating — but from a drug interaction standpoint, CBD is actually more potent than THC. CBD has been shown in pharmacology research to inhibit several CYP450 enzymes, including CYP3A4 and CYP2D6, which metabolize nearly 60% of all prescription medications.
Why CBD Interactions Are Common
CBD can:
- Slow down medication metabolism
- Increase medication levels in the bloodstream
- Intensify side effects
Enzyme Inhibition vs. Competition
- Competition means two substances use the same enzyme “lane.”
- Inhibition means CBD blocks the lane entirely, forcing medications to back up.
CBD is a strong inhibitor, which is why interactions can be significant. CBD affects the same enzymes that trigger grapefruit warnings on prescription bottles. If your medication says “avoid grapefruit,” you should be cautious with CBD.
Medications that may interact with CBD include:
- SSRIs, SNRIs, and tricyclic antidepressants
- Tricyclic antidepressants
- Beta‑blockers and blood pressure medications
- Anti‑seizure medications
- Opioids
- Statins
- Anticoagulants and blood thinners
CBD may increase medication levels in the bloodstream, potentially intensifying side effects. For example, CBD and SSRIs may increase drowsiness, while CBD and blood pressure medications may cause dizziness or low blood pressure.
If you’re considering CBD for anxiety, inflammation, or pain, speak with a certified medical marijuana doctor:
High-Risk Medications That Interact With Medical Marijuana
Some medications require extra caution when combined with cannabis due to their narrow therapeutic window or strong CNS effects.
1. Blood Thinners (Bleeding Risk)
Medications like warfarin rely on precise dosing. CBD and THC can slow their metabolism, potentially increasing bleeding risk.
2. Sedatives (Respiratory Depression Risk)
Benzodiazepines, opioids, and sleep medications already depress the central nervous system. Adding THC or CBD can intensify sedation and impair breathing.
3. Heart Medications
Beta‑blockers, calcium channel blockers, and antiarrhythmics can interact with cannabis, affecting heart rate, blood pressure, and rhythm stability.
4. Anti‑Seizure Drugs
CBD can raise levels of medications like clobazam or valproate, increasing side effects such as fatigue or liver strain.
Cannabis and Antidepressants: THC vs. CBD Effects
Many patients use cannabis alongside antidepressants such as SSRIs, SNRIs, or tricyclics. While cannabis may help with mood, anxiety, and sleep, combining it with antidepressants can produce:
- Increased sedation
- Changes in medication metabolism
- Heightened anxiety in some individuals (THC‑related)
- Reduced anxiety (CBD‑related)
Each class interacts differently:
- SSRIs/SNRIs: CBD may increase blood levels, potentially intensifying drowsiness or nausea.
- TCAs: THC may increase heart rate, which can compound TCA‑related cardiovascular effects.
CBD, in particular, can raise blood levels of certain antidepressants, making medical oversight essential.
THC vs. CBD for Anxiety
- THC can reduce anxiety at low doses but may increase anxiety at higher doses.
- CBD is generally calming and may help balance THC’s effects.
Serotonin‑Related Considerations
Cannabis does not directly cause serotonin syndrome, but combining high‑dose CBD with certain antidepressants may influence serotonin signaling. This is rare but worth monitoring.
Cannabis and Blood Pressure Medications
Cannabis — especially CBD — can lower blood pressure in some patients. When combined with:
- Beta‑blockers
- ACE inhibitors
- Calcium channel blockers
This may cause dizziness, lightheadedness, or fatigue. THC may temporarily increase heart rate, which can also affect cardiovascular medications.
Short‑Term Effects of Cannabis and Blood Pressure Meds
THC may temporarily increase heart rate and cause mild blood pressure drops.
CBD may lower blood pressure, especially in stressful situations.
Long‑Term Effects
Some patients experience improved cardiovascular stability with consistent cannabis use, but this varies widely.
Orthostatic Hypotension
Standing dizziness can occur when cannabis and blood pressure medications combine — especially in older adults.
Have questions about cannabis and your current medications? Our physicians can help you learn more.
Cannabis and Pain Medications: What are the Benefits and Risks
Many patients use cannabis alongside:
- Opioids
- NSAIDs
- Muscle relaxants
- Neuropathic pain medications (gabapentin, pregabalin)
Cannabis may reduce the need for opioids, but combining them can increase sedation. CBD may also alter how the liver processes certain pain medications.
Opioid‑Sparing Effect
Cannabis may reduce the amount of opioids needed for pain control — a major benefit for many patients.
Risks of Combining CNS Depressants
THC + opioids or muscle relaxants can increase sedation, impair coordination, and slow breathing.
Nerve Pain Medications
CBD may alter the metabolism of gabapentin or pregabalin, potentially increasing dizziness or fatigue.
Signs of Cannabis Drug Interactions to Watch For
Patients should watch for:
- Unusual drowsiness
- Dizziness or lightheadedness
- Nausea
- Heart rate changes
- Increased medication side effects
- Confusion or impaired coordination
If symptoms appear, contact a medical professional promptly.
FAQ: Medical Marijuana and Prescription Medication Interactions
1. Can medical marijuana interact with my prescription medications?
Yes. Both THC and CBD can alter how medications are metabolized, potentially making them stronger, weaker, or longer‑lasting. This is especially important for patients taking multiple prescriptions.
2. Should I stop my medication before using cannabis?
No. Never stop or change prescription medications without medical supervision. A doctor can help you adjust safely if needed.
3. How long should I wait between cannabis and medication?
Timing varies depending on the medication and cannabinoid. A medical professional can help determine safe spacing.
4. Is CBD safe to take with antidepressants?
CBD may increase blood levels of certain antidepressants, which can intensify side effects. Monitoring is important.
5. Can cannabis be used with blood pressure medications?
Yes, but both THC and CBD can affect blood pressure. Monitoring is important.
6. Does cannabis interact with pain medications?
Cannabis may enhance sedation when combined with opioids or muscle relaxants. CBD may alter metabolism of certain pain medications.
7. How do I know if cannabis is safe with my medications?
A certified medical marijuana physician can review your prescriptions and help you build a safe, personalized treatment plan.
Not sure if cannabis is safe with your medications? Speak with a certified medical marijuana doctor today.
Best Practices for Using Cannabis Safely With Medications
To use medical marijuana safely with prescription medications:
- Start low and go slow
- Keep a complete medication list
- Use consistent cannabis products
- Avoid mixing multiple new substances at once
- Track symptoms and side effects
- Consult a medical marijuana doctor regularly
Medical marijuana can be a valuable tool for managing pain, anxiety, and other conditions—but only when used thoughtfully alongside prescription medications. Because THC and CBD can affect how drugs are metabolized, personalized guidance is essential to avoid unwanted side effects or complications.
Ready to explore medical marijuana safely and confidently? Schedule your evaluation today.
A qualified physician can help you build a treatment plan that works with your medications—not against them.
This content, written by the editorial team at Marijuana Doctor, is for informational purposes only and does not constitute medical advice.